Main content
Platform for support and information about psychosis (vulnerability), trauma, mood problems and recovery
Read more about psychosisBlogs
-
Sleeping pills: Gateway to slumber or silent danger?
Sleeping pills, often sought as a remedy for insomnia, present complex challenges.
-
Psychological self-tests, a myth? In search of the real you
Psychological self-tests. The internet is full of them. Do you need these and do they provide some help?
-
Privacy and mental health, NL and UK
Privacy and mental health, an overview and some thoughts.
Learn more about psychosis
What is psychosis? What are the common symptoms, and what do we know about possible causes? Can you recover from it and how? Here we provide down to earth, useful information.
Latest
-
Check in on those around you – #YouAreNotAlone
At times, it can be obvious when someone is struggling to cope. But sometimes the signs are harder to spot. Check in on those around you....
-
I’m glad my mom died – Jennette McCurdy
I’m Glad My Mom died by Jennette McCurdy is an inspiring tale of resilience, independence and the joy of washing your own hair.
-
The Varieties of Spiritual Experience – David Yaden, Andrew Newberg
Spiritual experiences have occurred within people around the world and throughout history, up to and including the present day. Yup, but nowadays science tries to make...
Featured
-
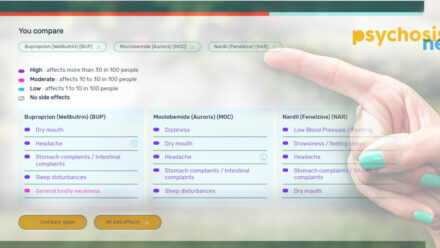
Compare antidepressants
You cannot predict in advance which drug will work best for you. Use this tool to compare antidepressants and their side effects.
-
About PsychosisNet
PsychosisNet.com is a Public Benefit Organisation founded by professionals, experience experts and others to offer clear & useful info, hope, and support.
-
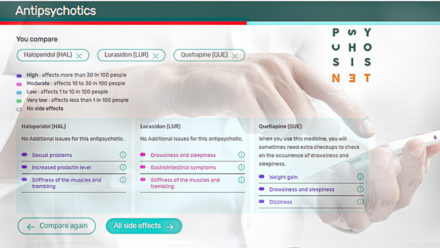
Compare antipsychotics
You cannot predict in advance which drug will work best for you. Use this tool to compare antipsychotics and their side effects.